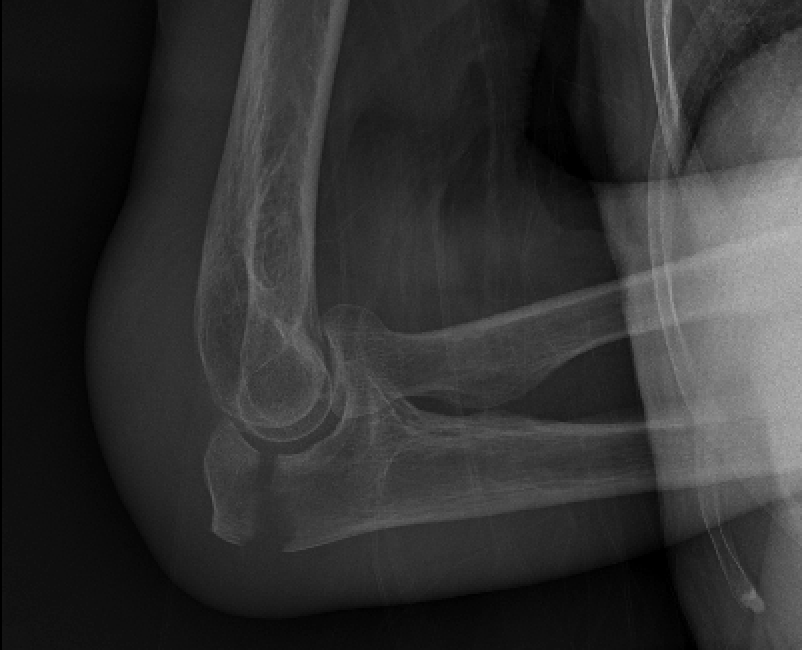
Olecranon fractures in the very elderly have surprisingly good outcomes without surgery, and can avoid a high risk of complications.
Continue readingAdvanced Physiotherapy now Available at BallaratOSM
We are very pleased to introduce the latest member of the BallaratOSM team, and announce the expansion of our services to provide patients of Ballarat and surrounding districts with the highest quality, patient-focused, individual care.
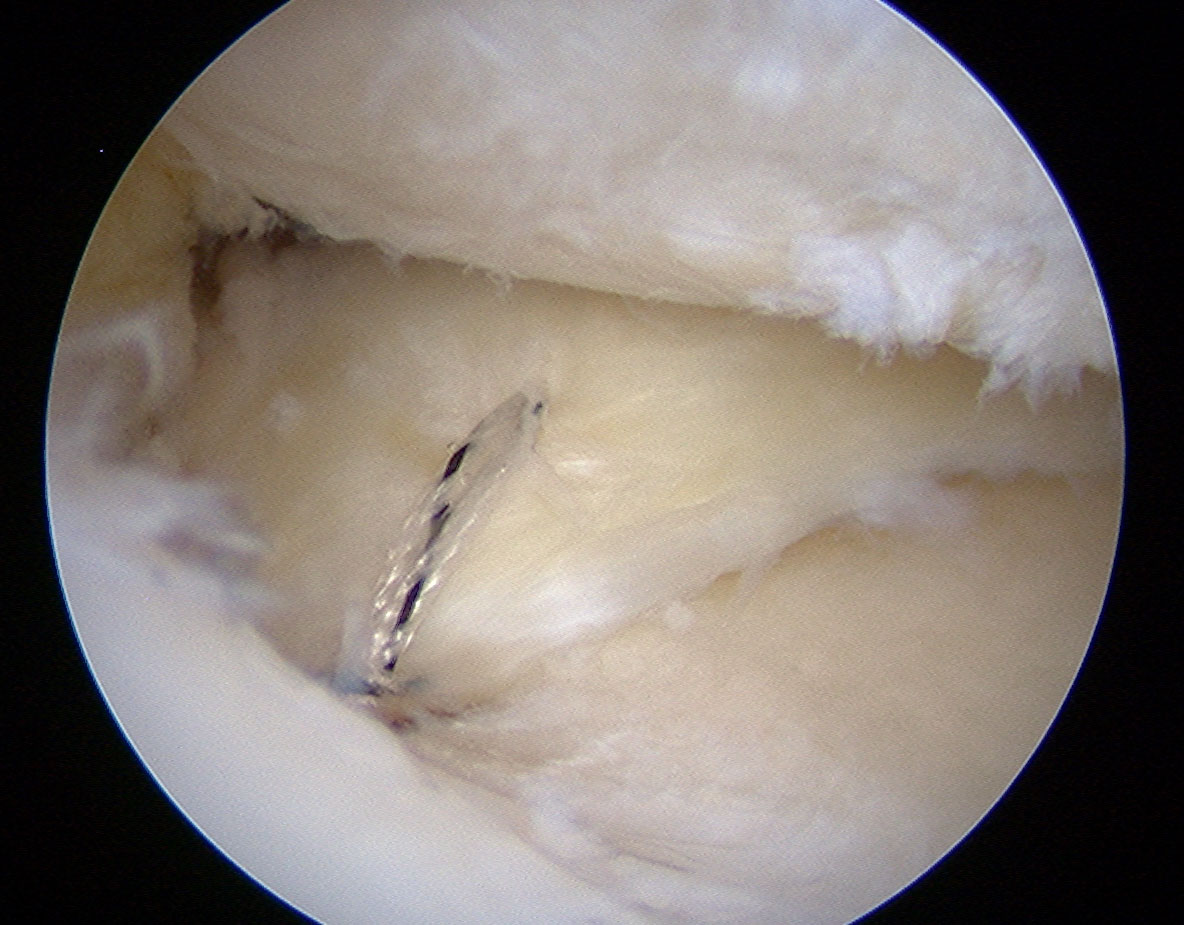
Continue readingMeniscal repairs have been under-utilised by surgeons
David Mitchell has been to the International Society of Arthroscopy, Knee Surgery, and Orthopaedic Sports Medicine biannual meeting, this time in Mexico.
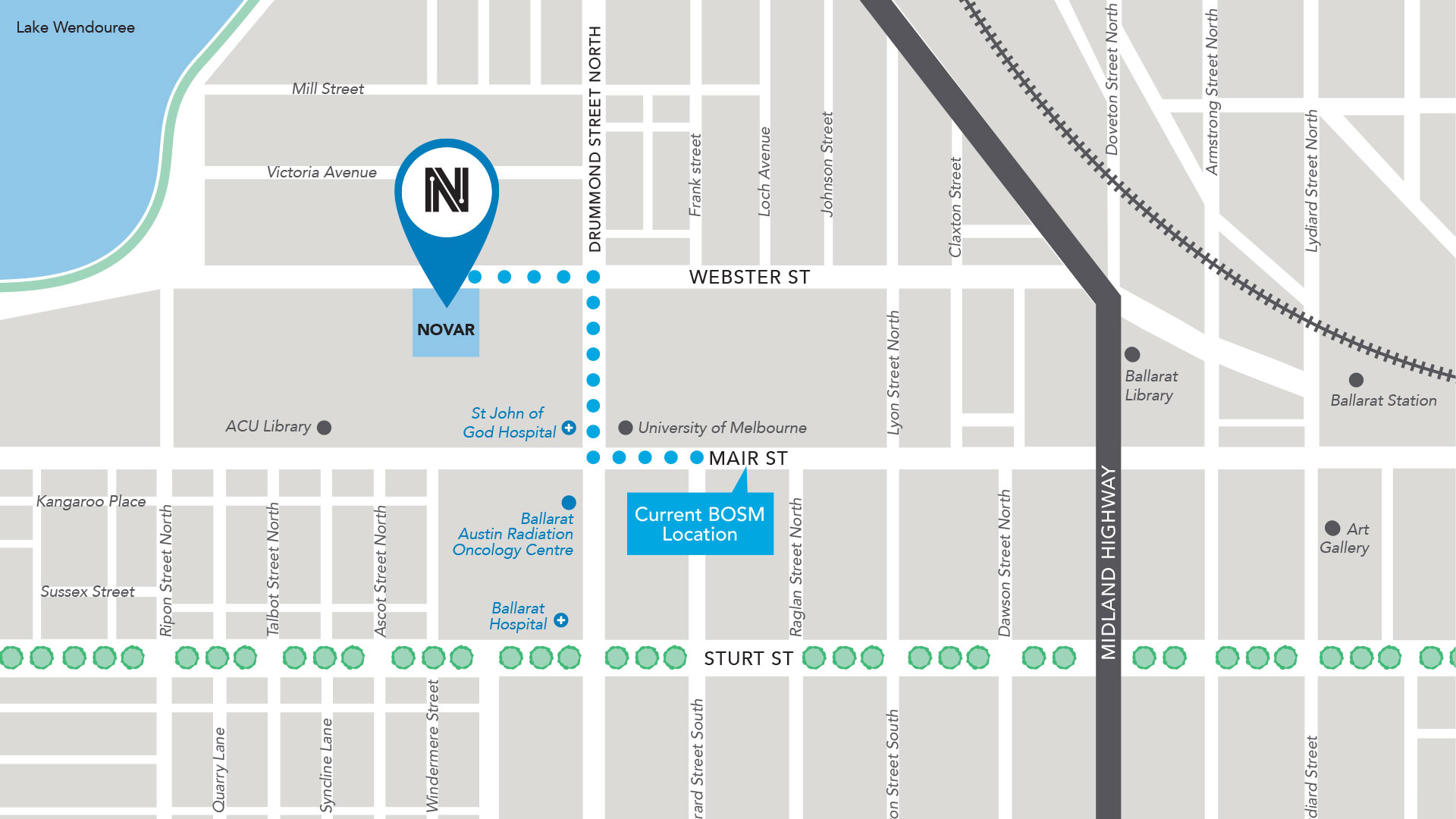
Continue readingWe Have Moved!
As of 29th April, we have moved to Novar at 109 Webster Street. All Orthopaedic consultations and Sports Medicine consultations will take place at the new address
Continue readingIf in doubt, sit them out
Tuesday 12 February saw the launch of the Concussion in Sport Australia Position Statement.
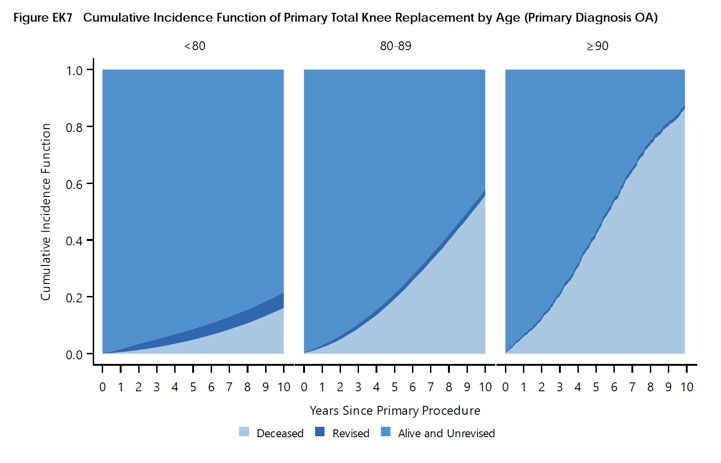
Continue readingJoint replacement “before they’re too old”?
The reason to have a joint replacement is pain or disability. If you don’t have much of either, the risk of surgery includes not making you better enough for it to have been worthwhile.
Continue reading6 Steps to add Ballarat OSM Appointment Page to your Mobile Device
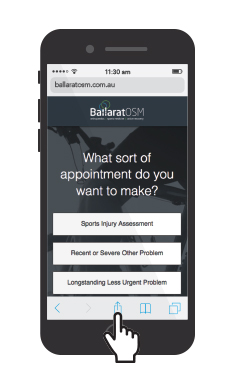
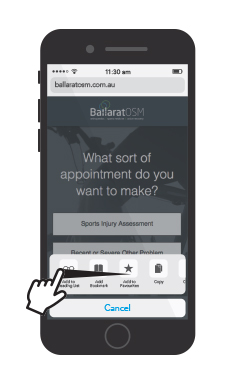
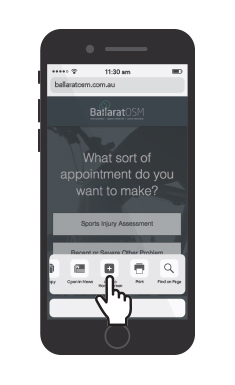
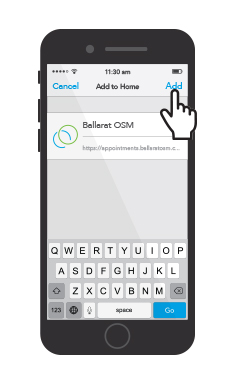
How to add the Ballarat OSM Appointment Page to your Mobile Device in 6 Easy Steps
Without having to continuously search through your internet browser and navigate our website, we have made it quicker and easier for you to book an appointment online from your mobile device. Here are 6 steps on how to add the Ballarat OSM appointment page to your mobile device.
The results are in on the ASPREE trial – and not what was expected
A study in Australia and the US was commenced almost a decade ago to assess whether being on long term aspirin increased a perfectly healthy patient’s chance of survival. Aspirin is traditionally expected to reduce cardiovascular disease such as heart attacks or strokes, there have been studies showing a reduced cancer risk, and only a tiny increase in bleeding risk causing death.
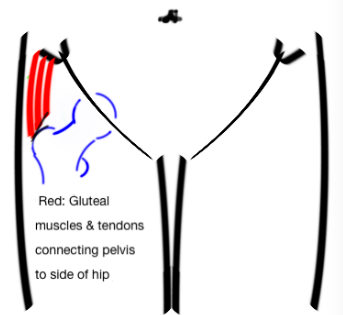
Continue readingThe paradigm of “trochanteric bursitis” has changed. The old days of cortisone are gone.
Patients present with pain over the outer aspect of their hip, it can radiate down as far as the knee. It is exacerbated by walking, and can be excruciating to lay on in bed. The pain seems to be caused by a tendinopathy of the gluteal tendons.
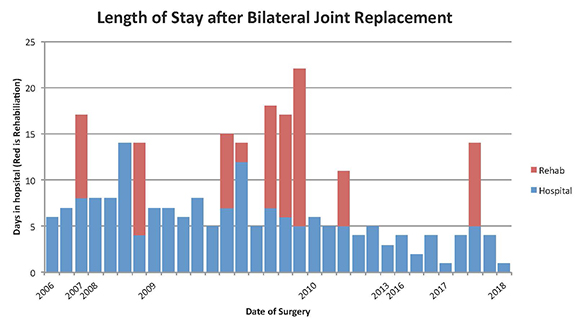
Continue readingUpdate on bilateral joint replacements
Patients having two joint replacements at the same time is a controversial question. In general, most patients are best to have a short hospitalisation, get out and get recovered from the first side, before embarking on the other.
Continue reading