Robotic knee replacement surgery has been widely available for some years – and in Ballarat at St John of God, we have three robots to use with three different companies total knee replacement, and some partial knee replacements. Our surgeons using it find it a useful tool streamlining the operation.
Continue readingSport’s Back! And so is Sports Med Teaching
Ballarat OSM supports local national basketball tournament
The team at Ballarat OSM have been out supporting Ballarat Basketball this week and providing Sports Medicine coverage at the Australian under 14 national club tournament here at the new Ballarat Sports and Events Centre.
We have been staffing the tournament with an elite team of Sports Medicine, Sports Physiotherapy and trainer professionals to take good care of athletes in Ballarat.
We have been treating players court side and managing their needs for efficient and high quality care that allows them to play at their best or recover quickest.
We strive to support athletes from and in the western district with our high quality, unique sports medicine team!
Luke Blunden
APA Sports and Exercise Physiotherapist
Travelling with an elite sporting team

Insights from the U19 FIBA World Cup Basketball with Ballarat OSM Sports and Exercise Medicine Registrar, Dr. Anthony Hipsley
One day before we leave Melbourne to fly to Latvia and Greece. The boys have their final training session and are looking great. Unfortunately, it’s never that easy…
When I was asked to be the Team Doctor for the Men’s U19 Australian Basketball Team on their upcoming tour to Europe for the FIBA World Cup, I immediately became both excited and nervous. I knew it would be a big job but a fantastic experience.
The key to a successful tour with an elite sporting team is preparation. Conducting thorough, yet practical medical screens of my athletes was an important first step. This allowed me to understand the past and present medical histories, as well as mitigate the risk of future injuries. It also gave me the opportunity to build rapport and educate the athletes about health and safety. Ensuring up to date vaccinations, providing health information and preparing your medical kit are other pre-tour tasks which require careful planning.
So what happened 24 hours before we jetted off to Europe? One of our best players pulls himself out of training with an acute hip injury. Not ideal timing! Needless to say, the coach is fretting, as are we all. Thankfully, we are able to get him an MRI within a couple of hours to help with diagnosis and guide treatment. A lengthy discussion follows between myself, physio, head coach and athlete about the way in which this injury might affect his ability to play 7 games against the world’s best competition. Always expect the unexpected when it comes to injuries – lesson learned.
Besides managing injury in sometimes inopportune moments, another vital aspect of being a Team Doctor on tour is optimising performance. I collected “wellness” data from the athletes, which gave me helpful information about sleep, muscle soreness, hydration and fatigue. If there was a downward trend, I engaged the athlete to rectify the issue before performance was jeopardised.
We travelled to Latvia and Greece with 17 people – 10 athletes and 7 supporting staff. It goes without saying that a Team Doctor in a foreign, high stakes environment must exhibit strong communication, organisational and decision making skills. However, I have come to learn of more inconspicuous skills that make life easier. Firstly, humour. On day 1, the head coach asked me, “Doc, what’s your favourite movie”, to which I (truthfully) replied, “Easy. Dumb and Dumber”. All I can say is, our relationship grew steadily from there. “So you’re telling me there’s a chance?” was quoted relentlessly. I also have come to realise the importance of looking after yourself. I exercise every day at home, so I try and do the same on tour. I think of this approach as controlling the controllables, in this case, my own wellbeing.
Travelling as a Team Doctor with an elite sporting team is challenging, yet incredibly rewarding. I take with me many lessons learned and lifelong memories. Alas, we didn’t achieve our goal of winning a medal in the 2019 FIBA World Cup Basketball Tournament, however there is always next time. So you’re telling me there’s a chance!!!
Dr. Anthony Hipsley
Sports Medicine Registrar
Ballarat OSM
What’s stopping you?
What’s Stopping You?
Exercise is good for you. We all know that, it’s been a constant public health message for years, like smoking is bad for you, and you should ‘Slip, Slop, Slap’ in summer. Most people even get the message that you should exercise for 30 minutes a day. But how many of us actually do it?
Australia is one of the fattest countries on earth, and getting fatter. Childhood obesity rates are increasing, and ‘lifestyle’ diseases like Type 2 diabetes are wreaking havoc on the health of not only people, but the country’s health budget. Governments publish strategies every few years, but the trends keep getting worse. So, what do we have to do to change this?
Broad-brush statements like those above are easy to agree with, but hard to know what to do with as an individual. So, I have two questions directly for you:
- Are you happy with how much you move and how you feel? And if not,
- What’s stopping you?
If the answer to question 2 is an injury, then let’s do something about it. Sports medicine physicians are expert at finding ways to rehabilitate injuries as best as possible. Sometimes this involves rest, but not for too long. Often it involves stretching, strengthening or other exercises, which can be performed with input from a physiotherapist, exercise physiologist or osteopath. It may involve other treatments such as injections, which can often be performed in the rooms. Occasionally it will require surgery, in which case a sports physician will know which surgeon is the best one to perform the operation.
If the answer is illness, lack of fitness or other limitation, a sports physician will know how to tailor an exercise program around your limits. Sports Physicians are medical specialists, and understand how illness affects exercise, and vice versa.
Or if the answer is not enough time, too much to do, I’m too tired and I can’t fit it into my life, a sports physician may just have some ideas on how to make that little bit of activity part of your day.
Are you active enough?
So what’s stopping you?
Dr Greg Harris
Sport and Exercise Physician
Ballarat OSM
Do Robots Improve Surgery?

The Australian Orthopaedic Association, the Australian Knee Society & the Arthroplasty Society of Australia have just published a position statement on robotic surgery. Meanwhile we continue to work hard on alignment and balance of knee replacement surgery.
We identify that the ZUK partial knee replacement at five years has a revision rate of 4.9%, the only registry data on robotic surgery is the Restoris with a rate of 1.2% at one year. We are awaiting further data.

The Narcotics problem and how ‘LIA’ solves It
The combination of Meloxicam, Paracetamol and Tramadol as a top up covers just about every scenario. For surgery – Local Infiltration Analgesia, or LIA (Ropivicaine, Ketorolac, Dexamethasone, and Adrenaline) is critical. Norspan (Buprenorphine 5ug/hr) for knee replacements, posterior approach to the hips seems to help and avoid peaks and troughs in pain control. A little Amitriptyline for rare neuropathic pain is useful. But I wonder whether the narcotics crowd has fanned the anxieties of prescribers, making narcotics the easy solution for doctors?
I accept that Tramadol is also potentially addictive, but I found a decade ago when I swapped using Endone to Tramal, that my patients no longer required another five boxes, but were likely to use just a bit over one box after knee replacement surgery. Tramal is much less addictive than Endone.
Some surgeons are preferring Tapentadol – although I wonder whether less serotonergic effect is actually better, and the fast acting option is not covered by the Pharmaceutical Benefits Scheme. Nausea is unlikely if the patients if the starting dose is 50mg at a time, and the patients actually have enough pain to justify it. Hallucinations do rarely occur, in which case we swap to something else.
Interaction with SSRI’s (Selective serotonin reuptake inhibitors) is rare – serotonin syndrome with normal doses of SSRIs or SNRIs (Serotonin and norepinephrine reuptake inhibitors) and normal doses of Tramal have not been observed by this author despite being used in hundreds of cases. The more depressed a patient is – the more they should avoid narcotics!
In the instance of joint replacement surgery – Torodol (ketorolac) is administer in the periarticular mix intra-operatively, and directly into the joint via a wound catheter with a 0.4um filter after surgery. The evening dose is for morning patient, the morning after dose is received by all patients. The Mobic (meloxicam) is used typically for three weeks for hip and knee replacements.
|
eGFR
|
Intraoperative
|
Evening
|
Morning
|
Discharge
|
|
>90
|
30mg Torodol
|
30mg Torodol
|
30mg Torodol
|
7.5 Mobic bd
|
|
60-90
|
30mg Torodol
|
30mg Torodol
|
30mg Torodol
|
7.5 Mobic bd
|
|
55-59
|
30mg Torodol
|
30mg Torodol
|
7.5 Mobic bd
|
|
|
30-54
|
30mg Torodol
|
7.5 Mobic daily
|
||
|
15-29
|
30mg Torodol
|
|||
|
<15
|
30mg Torodol
|
7.5 Mobic daily
|
We remeasured the eGFR in patients after surgery if their preoperative eGFR was abnormal. The graph below is of 63 patients who had a followup eGFR in the two years prior to February 2018. We note a dip in eGFR on day one after surgery, then recovery. We’ll collect more data and hopefully get it into a peer reviewed journal.
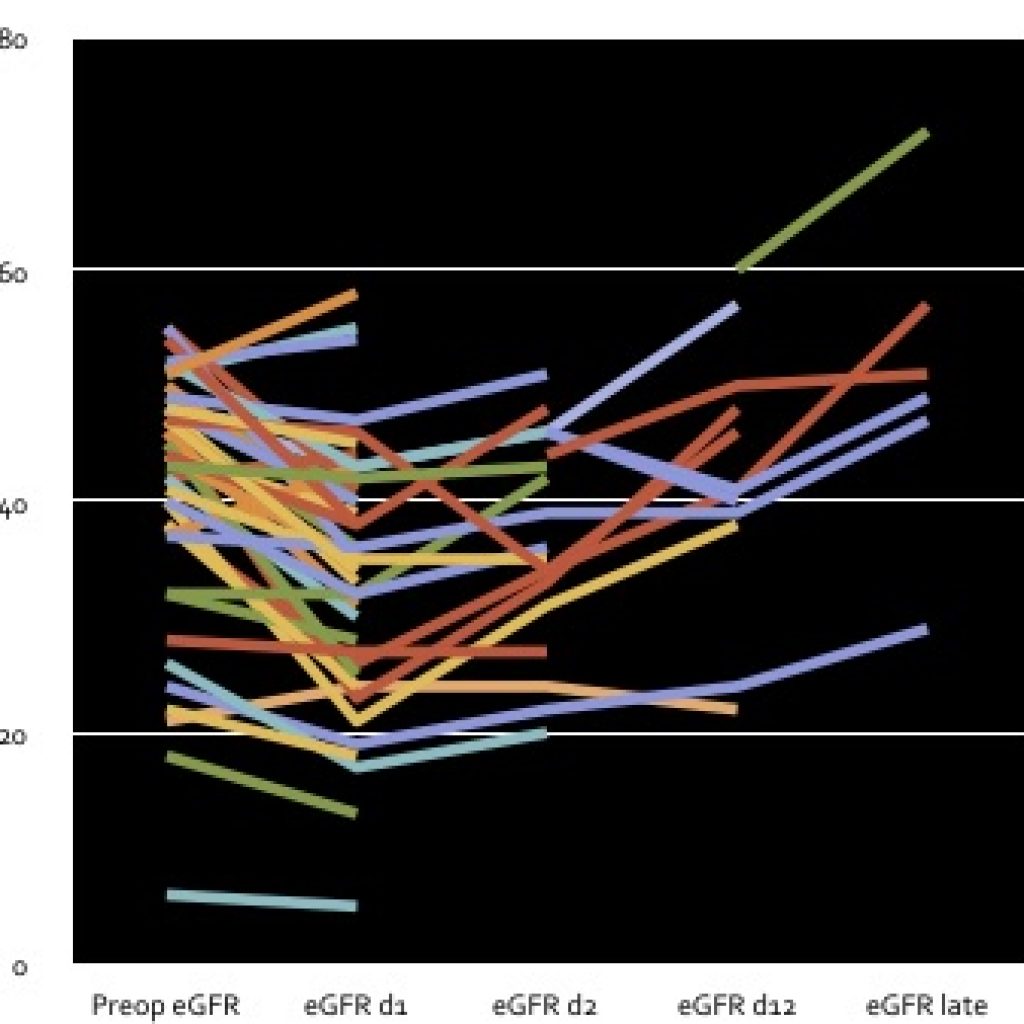
Orthopaedic Surgeon
Men’s Health Pub Clinic


Most people do not know how much they should weigh
The knee joint carries nine times your body weight as you use stairs. The hip uses 3.3x your body weight with every step. This is because of the amazing mechanics of the body, but it does have a downside – If you are overweight, you’re overworking your joints.

This graph shows with the green line, your maximum weight for a normal BMI. BMI’s are argued about for a general health point of view. Its is likely with a BMI of 30 you will still have a normal life expectancy, but your knee joint will not. Even if you’re 6’6, 198cm, your knee will eventually struggle if you weigh 100kg.
Some people do not accept the target weight based on their height and a BMI of 25, and come up with ten reasons why they can’t get to that weight But we would like you to have a target weight, and make a plan as to how to get there. The good news is that dropping 8 kilos for most people means the knee pain will improve. Some people will find that exercise and a small weight reduction fixes their knee pain, diabetes, hypertension, and cholesterol.
At the very least, being Strong, Supple and Slim will make you healthier.
If you’re serious about losing weight, you’ll need help. The Michael Mosley book – “The Fast 800” is an easy read plan as to how to lose weight. Mosley initially wrote about the 5:2 diet, this takes the idea further, but gives you a few more calories! You will need to calorie count at least two days per week. You should aim aim to introduce time restricted eating. It is easier if you enlist the help of your family and the people you usually eat with.

Mr David Mitchell
Orthopaedic Surgeon
References:
Mosley, Michael. The Fast 800. 2019. Simon and Schuster (Australia)
Brukner, Peter. 2018. “Fat Lot of Good”. How the experts got foot and diet wrong and what you can do to take back control of your health.”
What’s Cycling Got To Do With Orthopaedics?
Shaun English & David Mitchell have completed the 2019 Peaks Challenge!
This is a bike ride from Falls Creek, to Mount Hotham, Omeo, and back to Falls Creek.
11 hours 25 minutes (10 hours riding time) covered 235km, 4196 metres of climbing.
A tough day!

To do a cycling event like that you need:
- training
- planning
- dedication
- persistance
This is how we do Orthopaedic Surgery too!